Potential Health Benefits of Magnesium
Magnesium benefits include enhancing energy production, mood stabilization, sleep improvement, and constipation prevention, as well as relieving muscle aches and lowering the risk of cardiovascular disease. It also plays a crucial role in managing type 2 diabetes by improving symptoms and preventing its development, in addition to fighting inflammation.
- Boosts energy levels [1-4]
- Helps stabilize mood [5-13]
- Improves sleep quality [14-24]
- Prevents constipation [25-32]
- Relieves muscle aches and spasms [33-46]
- Lowers the risk of cardiovascular disease [47-58]
- Improves symptoms of type 2 diabetes and prevents its development [59-69]
- Fights inflammation [70-84]
Key Takeaways
- Magnesium serves as a crucial cofactor for over 300 enzymatic reactions in the body. These reactions are involved in various processes such as energy production, DNA and RNA synthesis, muscle function, and regulation of blood pressure.
- Magnesium plays a significant role in metabolic pathways, including those related to adenosine triphosphate (ATP) metabolism. It is essential for insulin metabolism, blood sugar regulation, and the synthesis of proteins.
- Adequate magnesium intake is associated with cardiovascular health. It helps regulate blood pressure, maintain normal heart rhythm, and has been linked to improved serum lipid profiles, potentially reducing the risk of cardiovascular diseases.
- Magnesium is crucial for the regulation of muscular contraction, including the heart muscle. It is involved in oxygen uptake, electrolyte balance, and can impact exercise performance. Magnesium deficiency may lead to muscle cramps and weakness.
- Magnesium is vital for bone health, working in tandem with calcium and vitamin D. It contributes to bone density and helps prevent conditions like osteoporosis, playing a crucial role in maintaining bone mineral density. A balanced intake of magnesium is essential for overall skeletal development and maintenance, ensuring that bone mineral density is optimized to support a strong and healthy framework.
What is Magnesium?
Magnesium is a versatile mineral serving as a cofactor in over 300 enzymatic reactions crucial for energy production, DNA and RNA synthesis, muscle function, and blood pressure regulation. Playing a key role in metabolic pathways, magnesium supports ATP metabolism, insulin regulation, and protein synthesis. Adequate magnesium intake is linked to cardiovascular health, helping regulate blood pressure and improve lipid profiles. Essential for muscle function, magnesium impacts oxygen uptake, electrolyte balance, and exercise performance, preventing issues like muscle cramps. Additionally, magnesium is vital for bone health, collaborating with calcium and vitamin D to maintain bone density and prevent conditions such as osteoporosis. A balanced magnesium intake is fundamental for overall skeletal development and maintenance.
How Magnesium Works
Magnesium operates as a vital mineral in the body, participating in over 300 enzymatic reactions critical for diverse physiological functions. Serving as a cofactor, magnesium facilitates these enzymatic processes, including energy production, DNA and RNA synthesis, muscle contraction, and blood pressure regulation. It plays a key role in metabolic pathways, supporting ATP metabolism, insulin regulation, and protein synthesis. Magnesium is essential for cardiovascular health, contributing to blood pressure regulation and improved lipid profiles. Additionally, it influences muscle function, impacting oxygen uptake and electrolyte balance, which is crucial for exercise performance. Moreover, magnesium collaborates with calcium and vitamin D for bone health, contributing to bone density and overall skeletal development.
Chemical Structure of Magnesium
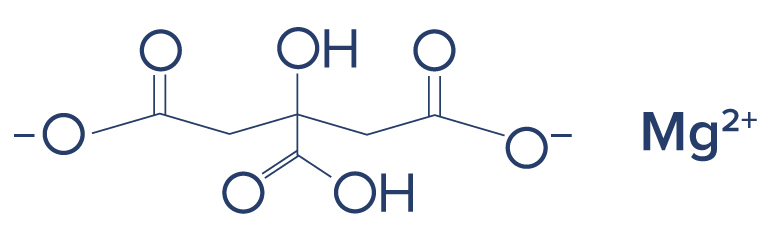
Research on Magnesium
A. Boosts Energy Levels

Magnesium boosts energy levels by playing a pivotal role in cellular energy production. It is a key component of ATP (adenosine triphosphate), the energy currency of the cell, involved in converting glucose into energy. By activating ATP, magnesium ensures that our cells have the fuel they need to perform bodily functions efficiently, from muscle contractions to nerve transmission. This essential mineral thus helps maintain high energy levels and supports overall vitality.
The energy-boosting properties of magnesium are backed by a number of studies:
- There is evidence that magnesium deficiency impairs exercise performance and enhances the negative consequences of vigorous physical activity. Based on dietary surveys and recent human experiments, increased intake of magnesium through diet or supplements has beneficial effects on exercise performance in magnesium-deficient individuals. [1]
- Studies show that Mg can enhance exercise performance by improving glucose availability in the brain, muscles, and blood, and reducing lactate accumulation in muscles. [2] Human studies have mainly examined physiological effects on diastolic blood pressure and systolic blood pressure, heart rate, and VO₂ max, but evidence also suggests a positive impact on muscle performance and strength. Intervention studies indicate that Mg supplementation can improve functional indices such as quadriceps torque, and in elderly women, it has been shown to enhance gait speed and chair stand time, highlighting its importance in both exercise performance and daily functional activities.
- Magnesium, the fourth most abundant mineral and a crucial intracellular divalent cation, plays a vital role in over 300 metabolic reactions in the body. It supports normal nerve and muscle function, heart rhythm, systolic and diastolic blood pressure, immune system, bone integrity, and regulates blood glucose levels while also enhancing calcium absorption. Given its significant involvement in energy production, muscle function, and glucose management, magnesium has been extensively researched as a performance enhancer for athletes. [3]
- A study investigated the effects of magnesium (Mg) on glucose and lactate dynamics in rats during and after exercise. [4] Pretreatment with magnesium sulfate significantly increased glucose levels approximately two-fold in muscle, blood, and brain during exercise compared to the control, indicating enhanced glucose availability. Furthermore, while lactate levels rose sharply in all areas during exercise in both groups, the Mg-treated rats showed a further increase in brain lactate during exercise and improved lactate clearance in muscle post-exercise, suggesting that Mg plays a crucial role in energy production and exercise performance by modulating glucose utilization and lactate clearance.
B. Helps Stabilize Mood

Magnesium improves mood by regulating neurotransmitters, which are chemicals in the brain that transmit messages between nerve cells and the brain. It plays a crucial role in the function of the nervous system and the regulation of the stress-response system. Magnesium’s ability to modulate the activity of the body’s stress-response system helps prevent the brain from becoming overstimulated, which can lead to anxiety, stress, and depression. Therefore, by maintaining adequate levels of magnesium, it can help stabilize mood, reduce stress levels, and contribute to overall emotional well-being.
Studies support the mood-enhancing effects of magnesium:
- Magnesium plays a crucial role in brain biochemistry and neuronal membrane fluidity, with deficiency linked to various neuromuscular and psychiatric symptoms, including depression. Despite mixed results regarding plasma/serum magnesium levels as indicators for depressive disorders, magnesium compounds are increasingly recognized for their therapeutic potential in treating not only depression but also migraines, alcoholism, asthma, heart diseases, and more. [5] Magnesium’s mechanisms as an antidepressant are not fully understood, but its impact on multiple systems related to depression development is acknowledged. Historical and contemporary research supports the efficacy and safety of magnesium supplementation, highlighting its significance in both conventional and homeopathic medicine as a treatment for mental health issues.
- A study investigated the impact of magnesium supplementation on depression in patients with magnesium deficiency, involving 60 individuals divided into two groups: one receiving magnesium oxide and the other a placebo for 8 weeks. [6] Results showed significant improvements in magnesium levels and depression scores, particularly in the magnesium group, where a notable reduction in the Beck Depression Inventory-II scores was observed compared to the placebo group. The findings suggest that daily intake of 500 mg magnesium oxide can effectively enhance depression status and correct magnesium deficiencies in depressed patients, indicating the importance of assessing and addressing magnesium levels in depression treatment.
- A study reviewed scientific literature from 2010 to March 2020 to assess the link between magnesium levels and various psychiatric disorders, including depression, anxiety, ADHD, autism, OCD, schizophrenia, and eating disorders, across 32 articles. [7] The findings indicate a notable association between low magnesium levels and depression, with some studies showing improvement in depressive symptoms following magnesium supplementation, either alone or in combination with antidepressants. However, the results regarding magnesium’s effectiveness and its plasma levels in other psychiatric conditions like anxiety, ADHD, and autism were mixed and less conclusive. Despite the variability in outcomes, the evidence suggests potential benefits from magnesium supplementation in managing psychiatric symptoms, underscoring the need for well-designed clinical trials to further explore magnesium’s therapeutic role and optimal use in psychiatric treatment.
- Major depression, a debilitating mood disorder, may not always respond well to antidepressants, which have been linked to increased suicide rates, especially among young people. [8] Magnesium deficiency, known to cause neuropathologies, exacerbates this issue as modern diets and water supplies often lack adequate magnesium, crucial for regulating neuronal calcium channels and nitric oxide production. Hypothesized as an effective treatment for major depression due to intraneuronal magnesium deficits caused by dietary insufficiencies, stress, and excessive dietary calcium, magnesium supplementation has shown rapid recovery in case histories. These findings suggest not only magnesium’s potential in treating depression and related mental health issues but also highlight the need for further research into magnesium deficiency as a public health concern, recommending the fortification of refined grain and water with magnesium to historical levels.
- A study investigated the link between dietary magnesium intake and depression among 8,894 US adults using data from the National Health and Nutrition Examination Survey (2007-2010). [9] Results revealed a statistically significant association between very low magnesium intake (less than 184 mg/day) and increased risk of depression, particularly in individuals younger than 65 years old. Conversely, in seniors, low magnesium intake appeared to have a protective effect against depression. These findings underscore the importance of magnesium in mental health and suggest age-specific impacts, highlighting the need for further research to understand the protective role of magnesium intake in older adults.
- A double-blind, randomized study on 32 women with premenstrual syndrome (PMS) assessed the impact of oral magnesium (Mg) supplementation on premenstrual symptoms. [10] Over two menstrual cycles, participants received either magnesium pyrrolidone carboxylic acid (360 mg Mg) or a placebo from the 15th day of their cycle until the start of menstruation. Results showed that magnesium significantly reduced total premenstrual distress as well as specific symptoms related to “pain” and “negative affect.” Additionally, significant increases in magnesium levels were observed in lymphocytes and polymorphonuclear cells but not in plasma and erythrocytes. These findings suggest magnesium supplementation as an effective treatment for mood-related PMS symptoms.
- An open-label, randomized, cross-over trial involving 126 adults with mild-to-moderate depression found that 6 weeks of magnesium chloride supplementation (248 mg of elemental magnesium per day) resulted in a significant improvement in depression and anxiety symptoms, with a net decrease in PHQ-9 and Generalized Anxiety Disorders-7 scores. [11] The study, conducted between June 2015 and May 2016, demonstrated high adherence rates (83%) and good tolerability, with 61% of participants expressing willingness to continue using magnesium supplements. The positive effects of magnesium on depression were observed within two weeks and were consistent across various demographic and clinical subgroups, suggesting magnesium’s potential as a fast-acting and well-tolerated treatment option for mild-to-moderate depression.
- In an 8-week randomized controlled study of individuals with low magnesium levels and severe stress, magnesium combined with vitamin B6 was found to significantly reduce stress more effectively than magnesium alone. [12] This secondary analysis focused on the impact of these supplements on depression, anxiety, and quality of life (QoL). Participants, all experiencing high stress as measured by the DASS-42 stress subscale, received either a combination of magnesium and vitamin B6 or magnesium alone. Results showed notable improvements in anxiety and depression scores for both groups, with a particularly rapid improvement within the first four weeks. Additionally, QoL enhancements were observed over the 8 weeks, with a more significant increase in perceived physical activity capacity in those taking both magnesium and vitamin B6. The study concludes that magnesium supplementation, both with and without vitamin B6, offers significant clinical benefits for individuals with stress and low magnesium levels.
- Sixty percent of clinical depression cases are considered treatment-resistant depression (TRD), with magnesium deficiency implicated as a significant factor due to its role in neuronal injury and neurological dysfunction, potentially manifesting as major depression. [13] Studies have shown that magnesium supplementation produces anti-depressant-like effects in animals, similar to strong anti-depressant drugs, and low cerebral spinal fluid and brain magnesium levels have been observed in patients with TRD and suicidal tendencies. Despite the historical and recent evidence supporting magnesium’s effectiveness in treating TRD, including a 2008 trial where magnesium was as effective as imipramine for depression in diabetics without side effects, comprehensive clinical trials are scarce. The removal of magnesium from processed foods and the addition of calcium, glutamate, and aspartate may exacerbate affective disorders. This evidence suggests that dietary magnesium inadequacy could be a primary cause of TRD, advocating for magnesium supplementation as a treatment, potentially benefiting nearly all individuals with depression.
C. Improves Sleep Quality

Magnesium improves sleep quality by regulating neurotransmitters involved in the sleep cycle, including increasing gamma-aminobutyric acid (GABA) levels in the brain, which promotes relaxation and stress reduction. Its role in maintaining healthy levels of GABA facilitates the transition to sleep and enhances the overall quality of sleep. Additionally, magnesium’s muscle-relaxing properties can alleviate physical discomfort, further contributing to a restful night’s sleep by reducing instances of nighttime awakenings and ensuring deeper, more restorative sleep phases.
A number of evidence supports the benefits of magnesium on sleeping problems:
- A systematic review aimed to explore the association between magnesium (Mg) intake and sleep patterns in adults by analyzing observational and interventional studies sourced from PubMed, Scopus, and ISI Web of Science up to November 2021. [14] Involving 7,582 subjects across 9 studies, it found observational evidence suggesting a positive link between magnesium status and sleep quality, such as reduced daytime sleepiness and longer sleep duration. However, randomized clinical trials (RCTs) presented mixed results, highlighting the need for more comprehensive trials to conclusively determine magnesium’s effect on sleep disorders.
- In a longitudinal study analyzing 3,964 participants from the CARDIA study, magnesium (Mg) intake was found to be marginally associated with improved sleep quality and significantly associated with reduced likelihood of short sleep duration (<7 hours), particularly among individuals without depressive disorders. [15] The study, which assessed dietary and supplementary Mg intake as well as the calcium-to-magnesium (Ca:Mg) intake ratio, found no significant association between Ca:Mg and sleep outcomes. These findings suggest a potential beneficial role of magnesium in promoting better sleep quality and longer sleep duration, highlighting the need for randomized controlled trials with objective sleep measures to further explore this relationship.
- In a double-blind randomized clinical trial involving 46 elderly subjects, magnesium supplementation was found to significantly improve various measures of insomnia compared to a placebo. [16] Over an 8-week period, subjects receiving 500 mg of magnesium daily experienced increases in sleep time, sleep efficiency, serum renin, and melatonin levels, along with decreases in the insomnia severity index (ISI) score, sleep onset latency, and serum cortisol concentration. These results suggest that magnesium supplementation could be an effective strategy to improve both subjective and objective insomnia parameters in the elderly, highlighting magnesium’s potential role in enhancing sleep quality and circadian rhythm regulation.
- A review analyzed three randomized control trials comparing oral magnesium supplementation to placebo in 151 older adults across three countries, using databases like MEDLINE and EMBASE. [17] The pooled analysis indicated a significant reduction in sleep onset latency by 17.36 minutes with magnesium supplementation, although the increase in total sleep time was not statistically significant. Despite the moderate-to-high risk of bias and the low to very low quality of evidence, the findings suggest that oral magnesium, being affordable and widely available, may offer some benefit for insomnia symptoms in older adults when taken in doses of less than 1 gram up to three times a day. The current literature’s quality, however, is insufficient for making well-informed clinical recommendations.
- In an experiment involving 100 adults with poor sleep quality, participants were assigned to receive either a 320 mg/day magnesium supplement or a placebo for seven weeks. [18] Initial assessments showed that 58% of participants consumed less than the recommended amount of magnesium, associated with higher BMI and plasma C-reactive protein (CRP) levels, indicating chronic inflammatory stress. While overall sleep quality improved for all participants, magnesium supplementation specifically increased serum magnesium levels in those with initial deficiency and decreased plasma CRP levels in participants with higher baseline inflammatory markers. These results suggest a link between low magnesium status and increased chronic inflammatory stress, potentially alleviated by magnesium intake. However, the improvement in sleep quality, regardless of supplementation, points to the need for further research to clarify the relationship between magnesium status and sleep quality.
- Using data from the Jiangsu Nutrition Study, which included 1487 adults, research indicated that higher dietary magnesium intake is associated with a reduced likelihood of experiencing daytime falling asleep among women, with an intake mean of 332.5 mg/day. [19] Despite these findings, no significant associations were observed between dietary magnesium consumption and other sleep disorder symptoms such as daytime sleepiness or snoring at night for either gender. The study highlights the potential gender-specific benefits of dietary magnesium in mitigating certain sleep disorder symptoms, underscoring the need for further investigation into the role of magnesium in sleep health at the population level.
- In a double-blind, placebo-controlled clinical trial conducted in a long-term care facility in Pavia, Italy, involving 43 elderly participants with primary insomnia, it was found that a nightly regimen of melatonin (5 mg), magnesium (225 mg), and zinc (11.25 mg) mixed with pear pulp significantly improved sleep quality over an 8-week period compared to a placebo. [20] The supplemented group showed notable improvements in sleep quality scores, ease of falling asleep, quality and restorative value of sleep, morning alertness, and quality of life, as measured by the Pittsburgh Sleep Quality Index, Leeds Sleep Evaluation Questionnaire, Short Insomnia Questionnaire, and SF-36, respectively. Total sleep time, assessed by a wearable sensor, also increased significantly, indicating that the combination of melatonin, magnesium, and zinc effectively enhances sleep and life quality in elderly individuals with primary insomnia.
- A study conducted a systematic review of clinical studies to investigate the relationship between serum magnesium (Mg) levels and obstructive sleep apnoea (OSA), revealing that OSA patients often have lower serum Mg levels compared to healthy controls, with a meta-analysis indicating a significant deficiency. [21] Although the mean serum Mg level in OSA patients falls within the normal range, the severity of OSA negatively impacts these levels, which tend to improve with OSA treatment. Additionally, low serum Mg levels in OSA patients are associated with increased systemic inflammation and cardiovascular risk, as evidenced by correlations with biomarkers like C-reactive protein and carotid intima-media thickness. These findings suggest that sleep deprivation linked to OSA may lead to Mg depletion, heightening the risk of cardiovascular and metabolic disorders.
- In a clinical trial involving 60 open-heart surgery candidates, magnesium supplementation significantly improved anxiety, depression levels, and sleep quality post-surgery. [22] Participants receiving 500 mg of magnesium oxide daily for five days showed higher magnesium levels, reduced anxiety and depression according to the Hospital Anxiety and Depression Scale (HADS), and better sleep quality based on the Petersburg Sleep Quality Inventory (PSQI), compared to the control group receiving routine care. These findings support the inclusion of magnesium supplements in post-operative care plans to enhance recovery outcomes related to psychological well-being and sleep in heart surgery patients.
- In an open clinical study involving 10 patients suffering from insomnia related to periodic limb movements during sleep (PLMS) or mild-to-moderate restless legs syndrome (RLS), oral magnesium therapy showed promising results. [23] Administered at a dose of 12.4 mmol in the evening for 4-6 weeks, magnesium significantly reduced PLMS associated with arousals and moderately reduced PLMS without arousal, while sleep efficiency improved notably. Especially in patients who reported improved sleep or RLS symptoms post-therapy, the effects of magnesium were more pronounced. This study suggests that magnesium treatment could be an effective alternative therapy for patients with mild or moderate RLS or PLMS-related insomnia, highlighting the need for further research on magnesium’s role in RLS pathophysiology and placebo-controlled studies.
- A study aimed at evaluating the efficacy of a magnesium-melatonin-vitamin B complex supplement in treating insomnia, 60 patients were divided into a study group and a control group. [24] The study group, treated with a daily dose of the supplement one hour before sleep for three months, showed a significant reduction in insomnia symptoms as measured by the Athens insomnia scale (AIS), with mean AIS scores decreasing from moderate to mild insomnia levels. In contrast, the control group remained at moderate insomnia levels. The findings suggest that a three-month regimen of Magnesium-melatonin-vitamin B complex supplementation can effectively reduce the severity of insomnia symptoms, demonstrating its potential as a beneficial treatment option for insomnia regardless of the cause.
D. Prevents Constipation

Magnesium prevents constipation by drawing water into the intestines, which softens the stool and makes it easier to pass. This process, known as osmosis, increases stool bulk and encourages bowel movements. Additionally, magnesium helps relax the muscles in the intestinal wall, improving gut motility and further aiding in the elimination process. As a result, adequate magnesium intake is essential for maintaining regular bowel movements and preventing constipation.
Studies show that magnesium is beneficial for gut health:
- Magnesium oxide has long been utilized as a laxative in East Asia based on empirical knowledge, with recent years seeing a revival in interest due to its convenience, low cost, and safety. [25] However, emerging clinical evidence suggests the need for careful consideration of dosage, serum concentration, potential drug-drug interactions, and side effects, particularly in the elderly and those with renal impairment. This review aims to assess the evidence for magnesium oxide’s use in treating constipation, offering a balanced guide to its benefits and limitations.
- In a randomized, double-blind placebo-controlled study conducted in Japan, magnesium oxide (MgO) was evaluated for its effectiveness in treating chronic constipation (CC) among 34 female patients. [26] The study found that MgO significantly improved overall improvement, spontaneous bowel movements, stool form, and colonic transit time over a 28-day period compared to a placebo. Although MgO did not significantly enhance complete spontaneous bowel movement response rates, it notably improved quality of life related to constipation. This demonstrates MgO’s efficacy as a treatment for CC in patients with mild to moderate symptoms.
- A study explored the relationship between dietary magnesium intake and chronic constipation using data from the 2007-2010 NHANES, including 9,519 participants aged ≥20 years. [27] It found that higher dietary magnesium intake was inversely associated with chronic constipation when defined by stool frequency, particularly among men, indicating a potential beneficial effect of magnesium on bowel health. However, no significant link was observed when constipation was defined by stool consistency. The findings suggest that increasing dietary magnesium might reduce the prevalence of chronic constipation, emphasizing the need for further longitudinal studies to confirm these results.
- A prospective, double-blinded randomized control trial involving 100 children with spastic cerebral palsy (sCP) and chronic constipation demonstrated that oral magnesium sulfate significantly improved constipation symptoms, stool frequency, and consistency compared to a placebo. [28] After a month of treatment, 68% of children in the magnesium sulfate group showed effective, safe relief from constipation versus 9.5% in the placebo group. This intervention also resulted in a noticeable reduction in the time mothers spent assisting with bowel evacuations, highlighting oral magnesium sulfate’s potential to not only alleviate constipation in children with sCP but also to reduce the caregiving burden.
- Functional constipation (FC), a chronic condition without identifiable physiological or anatomical causes, significantly affects quality of life and healthcare costs. [29] Traditionally managed through increased physical activity and dietary adjustments in fiber and water intake, FC often requires medication when these measures fail. Magnesium sulfate, known for its laxative properties and used in magnesium sulfate-rich mineral waters for centuries, has been widely recognized for its effectiveness. Despite its historical use, clinical studies on its efficacy in FC were scarce until the 21st century. Recent reviews of clinical data on magnesium sulfate-rich natural mineral waters have highlighted their potential as a safe, natural treatment option for FC, underscoring their efficacy and safety.
- In a trial involving 64 geriatric long-stay patients aged 65 years or older, all of whom were previously using laxatives, magnesium hydroxide was found to be more effective than bulk-laxative in treating constipation. [30] Patients taking magnesium hydroxide experienced more frequent bowel movements and required less additional laxative support compared to those on bulk-laxative, with more normal stool consistency observed during magnesium hydroxide treatment. Although two patients showed elevated serum magnesium levels, no clinical signs of hypermagnesemia were reported, suggesting magnesium hydroxide’s efficacy and relative safety for constipation relief in elderly patients.
- In the first prospective, double-blinded, randomized, placebo-controlled trial comparing a stimulant laxative (senna) and an osmotic agent (magnesium oxide [MgO]) in treating chronic idiopathic constipation, both senna and MgO demonstrated significant efficacy over placebo. [31] Enrolled participants, predominantly women with a long history of constipation, showed marked improvements in overall symptom relief, spontaneous bowel movements, complete spontaneous bowel movements, and quality of life related to constipation, with no severe treatment-related adverse events reported. This study highlights the effectiveness of both senna and MgO as treatment options for chronic constipation, indicating their potential to improve bowel function and patient well-being significantly.
- In an open-label study comparing magnesium (Mg)-enriched formula with a control formula for treating functional constipation in infants ≤6 months old, the Mg-enriched formula significantly improved stool consistency and frequency. [32] Within just 7 days, a greater proportion of infants fed with the Mg-rich formula experienced normal stool consistency and an increased daily stool frequency compared to those on the control formula. By the end of the study, parents reported high satisfaction with the Mg-enriched formula, with the majority expressing willingness to continue its use, demonstrating its effectiveness and parental approval in managing infant constipation.
E. Relieves Muscle Aches and Spasms

Magnesium helps relieve muscle aches and spasms by acting as a natural calcium blocker, which helps muscles relax. When magnesium levels are adequate, muscles can contract and relax properly, preventing cramping and spasms. Additionally, it aids in the transportation of calcium and potassium ions across cell membranes, a process essential for normal muscle function, nerve impulse conduction, and maintaining normal heart rhythm. This mechanism is why sufficient magnesium intake is crucial for preventing and alleviating muscle discomfort.
The benefits of magnesium on muscle aches and spasms are supported by several studies:
- Magnesium supplementation does not significantly reduce the frequency or intensity of skeletal muscle cramps in older adults, suggesting it may not be an effective preventative treatment for this group. [33] However, the effectiveness of magnesium for pregnancy-associated leg cramps remains uncertain due to conflicting research findings, indicating a need for further studies in this specific population.
- Muscle cramps, characterized by sudden, painful contractions of skeletal muscle fibers, can occur idiopathically or be associated with neuromuscular diseases, systemic disorders, and electrolyte imbalances, notably hypomagnesemia. [34] Magnesium plays a critical role in nerve transmission and muscle contraction, suggesting potential benefits for preventing or treating cramps. Despite its marketing as a prophylactic measure and experimental evidence suggesting improved exercise performance through enhanced glucose uptake and reduced lactate accumulation, the effectiveness of magnesium supplementation in cramp management remains uncertain.
- In a double-blind study, magnesium supplementation (350 mg daily for 10 days) significantly reduced muscle soreness among college-aged male and female subjects and showed a positive impact on performance, including total repetitions to failure at varying intensities. [35] Subjects reported lower levels of soreness on a 6-point scale post-supplementation, with improved perceptual responses regarding exertion and recovery compared to the placebo group. While performance improvements approached significance, the study indicates magnesium’s potential to enhance recovery and reduce muscle soreness.
- A study found that magnesium supplementation (350 mg daily for 10 days) significantly reduced muscle soreness and enhanced perceptual recovery in college-aged participants, compared to a placebo group. [36] These findings were accompanied by notable, though not statistically significant, improvements in performance metrics such as repetitions to failure at various percentages of the participants’ one-repetition maximum. Overall, magnesium showed potential benefits for both reducing muscle soreness and improving exercise performance, highlighting its value in sports nutrition and recovery strategies.
- A crossover randomized double-blind placebo-controlled trial conducted in Buenos Aires, Argentina, aimed to assess the efficacy of magnesium for treating nocturnal leg cramps but found no significant difference between magnesium and placebo treatments in reducing the number, duration, severity, or sleep disturbances caused by leg cramps. [37] Despite a total of 42 patients completing the study, which involved administering 900 mg of magnesium citrate twice daily for one month, all patients showed improvement over time, suggesting the observed benefits were likely due to natural progression, regression to the mean, or placebo effects rather than the magnesium treatment itself.
- A case report from a pediatric intensive care unit at a tertiary care, university-based children’s hospital detailed the successful use of intravenous magnesium sulfate to control muscle spasms and severe generalized rigidity in a 12-year-old child with moderate to severe tetanus. [38] This approach allowed for the avoidance of prolonged deep sedation, mechanical ventilation, or neuromuscular blockade. The treatment with magnesium sulfate showed significant improvement in the patient’s condition without any adverse effects, suggesting magnesium sulfate as a viable option for managing tetanus-induced muscle spasms and rigidity, with the caveat of close monitoring of the patient’s neurologic, cardiovascular, and respiratory status.
- A randomized, double-blind, cross-over placebo-controlled trial investigated the effectiveness of magnesium citrate in treating nocturnal leg cramps in non-pregnant individuals. [39] Participants received magnesium citrate equivalent to 300 mg of magnesium and a matching placebo for 6 weeks each. The study found a trend towards fewer cramps during magnesium treatment compared to placebo, with a significant number of subjects perceiving magnesium as helpful. Although there was no significant difference in the severity and duration of cramps between the treatments, the findings suggest that magnesium may be an effective treatment option for nocturnal leg cramps, warranting further evaluation. Diarrhea was noted as a side effect of magnesium citrate.
- A study explored the association between chronic musculoskeletal pain (CMP) and cardiovascular disease (CVD), identifying older age, female sex, hypertension, and calcium supplement use as factors linked to increased CMP intensity among CVD patients. [40] Additionally, the efficacy of Ice Power Magnesium In Strong Cream in alleviating muscle cramp pain in the lower extremities was evaluated. Results from 396 outpatients showed significant associations between the aforementioned factors and CMP intensity, while a separate analysis of 73 patients with muscle cramps demonstrated that the cream significantly reduced pain scores over 4 weeks. This indicates that specific demographic and health-related factors can influence CMP severity in CVD patients, and that topical magnesium cream is effective in treating muscle cramps.
- A review of four randomized controlled trials involving 332 pregnant women investigated the efficacy of magnesium supplementation for leg cramps during pregnancy, a symptom affecting 30%-50% of pregnant women. [41] The analysis, which included data up until July 2, 2020, found that magnesium supplementation did not significantly reduce the frequency of leg cramps, improve recovery from leg cramps, or produce significant side effects compared to a control group. The weighted mean difference for the frequency of post-treatment leg cramps and the odds ratios for recovery and side effects indicated that oral magnesium supplementation is ineffective in treating pregnancy-related leg cramps.
- A double-blind, placebo-controlled randomized trial on 46 older adults suffering from rest (nocturnal) cramps assessed the efficacy of a 5-day intravenous magnesium sulfate infusion in reducing leg cramp frequency. [42] Despite overcoming the oral bioavailability limitations of magnesium, the treatment did not significantly decrease the number of weekly cramps compared to the placebo, with no correlation found between magnesium retention and treatment response. This suggests that magnesium therapy, despite its popular marketing, may not be an effective treatment for rest cramps in the geriatric population.
- A 25-year-old paraplegic man, suffering from a severe and painful spasm in the left hamstring muscle group that resulted in extreme knee flexion, experienced immediate relief after receiving an intravenous injection of 2 g magnesium sulphate. [43] This case, following a T3/T4 vertebral compression fracture sustained three years earlier, highlights magnesium’s potential therapeutic effects on muscle spasms, inviting further discussion on the mechanisms through which magnesium operates to alleviate such conditions.
- A double-blinded, randomized, placebo-controlled trial involving 86 pregnant women with frequent leg cramps assessed the efficacy of oral magnesium bisglycinate chelate (300 mg per day) over a 4-week period. [44] The study found that magnesium supplementation significantly reduced both the frequency (86% vs. 60.5%, P=0.007) and intensity (69.8% vs. 48.8%, P=0.048) of pregnancy-induced leg cramps compared to placebo, without notable side effects like nausea and diarrhea. These findings suggest that oral magnesium could be a viable treatment option for managing leg cramps in pregnant women.
- A systematic review of seven randomized controlled trials (RCTs), including 361 participants, assessed the effectiveness of magnesium in treating nocturnal leg cramps (NLC) compared to placebo. [45] While magnesium therapy showed a slight effect in reducing leg cramps per week among pregnant women, it did not significantly affect the general population. Gastrointestinal side effects were slightly more common with magnesium than with placebo, but the overall evidence strength was considered weak due to small study sizes and short follow-up periods. The findings suggest that magnesium may have a modest benefit for pregnant women with NLC, though further, better-designed RCTs are needed.
- In a counterbalanced, double-blind, placebo-controlled, cross-over study involving nine male recreational runners, magnesium supplementation (500 mg/day for 7 days) prior to a 10 km downhill running time trial showed beneficial effects on inflammation and recovery post-exercise. [46] Magnesium intake significantly reduced interleukin-6 levels, indicating less inflammation, and improved recovery of blood glucose and muscle soreness, compared to the placebo. However, there were no significant differences in exercise performance, glucose and lactate levels during the time trial, or in creatine kinase levels and maximal muscle force post-exercise, suggesting that while magnesium may aid in recovery aspects, it does not enhance performance or functional recovery measures directly.
F. Lowers the Risk of Cardiovascular Disease
Magnesium plays a pivotal role in cardiovascular health by supporting the normal function of the heart, regulating blood pressure, and maintaining the balance of electrolytes. It helps to prevent the buildup of plaque in the arteries, reducing the risk of atherosclerosis and subsequently lowering the likelihood of heart attacks and strokes. Additionally, magnesium’s ability to improve blood flow and oxygen delivery throughout the body contributes to overall heart health and reduces the risk of cardiovascular disease.
- Magnesium, a vital intracellular cation, is crucial for cellular function, enzyme activity, and energy production, especially in the heart where it influences cardiac conduction and contraction by regulating ion channels. [47] It also plays a significant role in vascular health by affecting vascular tone and the process of atherogenesis, thus impacting the development of cardiovascular disease. Kidney disorders can affect magnesium levels, influencing cardiovascular risk. While observational studies link low magnesium with higher cardiovascular disease risks, supplementation trials have shown mixed results, leading to no general recommendation for magnesium supplementation in the absence of proven or suspected hypomagnesemia related to cardiac arrhythmias.
- Magnesium, a key cation in the human body, is integral to many processes crucial for cardiovascular health, including the regulation of vascular smooth muscle tone, endothelial function, and myocardial excitability. [48] It plays a pivotal role in the development and management of various cardiovascular disorders, such as hypertension, atherosclerosis, coronary artery disease, heart failure, and arrhythmias. The review highlights magnesium’s vasodilatory, anti-inflammatory, anti-ischemic, and antiarrhythmic effects, underscoring its importance in both preventing and treating cardiovascular diseases.
- Magnesium (Mg) is crucial for human health, with studies showing that higher Mg intake is linked to a reduced risk of cardiovascular diseases (CVD), including metabolic syndrome, diabetes, hypertension, stroke, and coronary heart diseases. [49] This review synthesizes evidence from epidemiological studies, randomized controlled trials (RCTs), and meta-analyses, highlighting the protective role of dietary and circulating magnesium against major cardiovascular risk factors and CVDs. The findings suggest that magnesium plays a significant role in cardiovascular health, with further research needed to explore its potential benefits in preventing CVD deaths and other cardiovascular conditions.
- A systematic review and meta-analysis examining the relationship between magnesium levels and cardiovascular disease (CVD) risk found that higher circulating magnesium levels are linked to a significantly lower risk of CVD and showed a trend towards reduced risks of ischemic heart disease (IHD) and fatal IHD. [50] While dietary magnesium did not show a significant overall association with CVD risk, it was associated with a lower risk of IHD, particularly up to a dietary intake threshold of approximately 250 mg/day. These findings underscore the potential protective effects of magnesium against heart disease and highlight the importance of further clinical trials to explore magnesium’s role in CVD prevention.
- Magnesium is a vital mineral involved in over 300 enzymatic reactions, crucial for blood pressure regulation, glycemic control, and lipid peroxidation, making it essential for cardiovascular health. [51] Despite its abundance in many foods and availability as a supplement, low magnesium intake in industrialized Western countries often leads to a high prevalence of magnesium deficiency, thereby increasing the risk of cardiovascular events and death. This article reviews the impact of magnesium deficiency on the cardiovascular system, highlighting the importance of maintaining adequate magnesium levels for heart health.
- Magnesium intake ranging from 500 mg/d to 1000 mg/d may lower blood pressure by up to 5.6/2.8 mm Hg, though clinical studies show varying results, with some indicating no change in blood pressure. [52] A combined dietary approach that increases magnesium and potassium while decreasing sodium intake proves more effective for blood pressure reduction, often matching the efficacy of antihypertensive medications. Magnesium enhances the effectiveness of all classes of antihypertensive drugs and may improve conditions like insulin sensitivity, hyperglycemia, diabetes, left ventricular hypertrophy, and dyslipidemia. While it’s yet to be definitively shown that magnesium intake can prevent or treat cardiovascular diseases, preliminary evidence and its roles as a natural calcium channel blocker and vasodilator suggest potential benefits in managing hypertension and improving cardiovascular health.
- A review highlights the significant role of increased dietary magnesium in protecting against diabetes, metabolic syndrome, hypertension, and cardiovascular diseases by improving insulin resistance, lipid profiles, and reducing inflammation, endothelial dysfunction, oxidative stress, and platelet aggregability. [53] Magnesium’s benefits are attributed to its actions as a calcium antagonist on vascular smooth muscle and its involvement in energy metabolism and various cellular functions. Despite the strong biological rationale for magnesium’s impact on health, prospective studies show only modest effects on preventing pathologies, and supplementation studies yield inconsistent results. The modest in-vivo role of magnesium deficiency, potential confounding by reverse causality, and the association with other beneficial nutrients suggest that the observed health benefits might be influenced by broader dietary patterns and health-conscious behaviors.
- A wealth of experimental, epidemiological, and clinical studies suggests a critical role for magnesium (Mg2+) in cardiovascular diseases, linking hypomagnesemia with electrolyte imbalances and various heart conditions, including ischemic heart disease and congestive heart failure. [54] Magnesium deficiency contributes to cardiovascular pathology through mechanisms like vasoconstriction of coronary vessels, increased intracellular calcium levels, oxidative stress, and alterations in cardiac cell membrane permeability. Additionally, magnesium’s interaction with calcium plays a pivotal role in myocardial contractility, influencing the heart’s response to stimulants and ischemic stress, particularly in the aged myocardium. Despite the ongoing debate over some mechanisms and the need for further research, the evidence supporting magnesium’s protective role in reducing cardiovascular disease morbidity and mortality is compelling, highlighting the potential benefits of magnesium supplementation in cardiac health management.
- An article provided an overview of magnesium research, detailing its historical development, the effects of magnesium on cardiovascular disease through basic and clinical studies, and the current magnesium intake levels in Japan as of 2002. [55] Basic research has shown that magnesium deficiency can reduce ATPase activity, leading to increased intracellular calcium in blood vessels and subsequent cardiovascular system vasoconstriction. Clinical studies have found significantly lower serum magnesium levels in patients with ischemic heart disease. Furthermore, the National Nutrition Survey in Japan indicated that the magnesium intake among males and females aged 15-49 years falls below the country’s recommended dietary allowances, highlighting a potential area of concern for public health.
- A dose-response meta-analysis of over 1 million participants across 40 prospective cohort studies investigated the impact of dietary magnesium intake on cardiovascular disease (CVD), type 2 diabetes (T2D), and all-cause mortality, revealing mixed results. [56] While no significant link was found between magnesium intake and total CVD or coronary heart disease (CHD), increased magnesium intake was associated with a lower risk of heart failure (22% reduction), stroke (7% reduction), T2D (19% reduction), and all-cause mortality (10% reduction). These findings suggest that enhancing dietary magnesium could potentially offer protective benefits against certain health conditions, underscoring the importance of magnesium in dietary recommendations.
- Magnesium, a crucial yet often neglected electrolyte, participates in over 300 enzymatic reactions including energy metabolism, glucose utilization, and cellular ionic balance. Its deficiency is increasingly common due to factors like poor diet and diuretic use, particularly among the elderly. [57] Associated with various conditions such as hypertension, heart failure, diabetes, and preeclampsia, clinical studies suggest magnesium supplementation can offer significant benefits. Addressing magnesium deficiency involves not only supplementation for those at risk or exhibiting symptoms but also identifying and correcting underlying causes, highlighting the importance of magnesium in maintaining overall health and preventing disease progression.
- In a comprehensive study involving 86,323 women from the Nurses’ Health Study, the relationship between dietary and plasma magnesium levels and the risk of coronary heart disease (CHD) was examined. [58] Despite finding no significant association between magnesium intake and total or nonfatal CHD, an inverse relationship was observed between dietary magnesium intake and fatal CHD, suggesting that higher magnesium consumption could reduce the risk of fatal CHD, potentially through mechanisms related to hypertension management. However, plasma magnesium levels, while lower in CHD cases, did not show an independent association with CHD risk when considering other cardiovascular biomarkers. This indicates that while dietary magnesium may not influence overall CHD incidence, it could play a role in decreasing the risk of fatal outcomes in CHD, possibly mediated by its effects on blood pressure.
G. Improves Symptoms of Type 2 Diabetes and Prevents its Development

Magnesium improves symptoms of Type 2 diabetes by enhancing insulin sensitivity and glucose control, contributing significantly to blood sugar control. It participates in the metabolism of sugar, helping to regulate blood glucose levels. Adequate magnesium levels facilitate the action of insulin, making it easier for the body to manage its blood sugar levels effectively. This can lead to improved glycemic control and a reduced risk of diabetes-related complications, making magnesium supplementation beneficial for individuals with Type 2 diabetes or those at risk for developing the condition.
- Magnesium deficiency is common in individuals with diabetes mellitus, influenced by factors such as glucosuria-induced loss, dietary inadequacies, and hyperinsulinemia. [59] While magnesium supplementation has been shown to improve insulin sensitivity and secretion in Type 2 diabetes patients, it has not demonstrated a significant impact on glycemic control in either Type 1 or Type 2 diabetes. However, in animal models, magnesium supplementation has been effective in reducing the onset of Type 2 diabetes. Moreover, lower plasma magnesium levels have been associated with severe retinopathy and higher blood pressure, although evidence on blood pressure reduction is inconclusive. These findings highlight the potential role of magnesium in preventing Type 2 diabetes, retinopathy progression, and managing hypertension, warranting further research.
- Oral magnesium supplementation has been shown to positively affect glucose metabolism and insulin sensitivity in individuals with diabetes or those at high risk of developing the condition. [60] Research comparing magnesium supplementation to placebo found that magnesium effectively reduces fasting plasma glucose in diabetic patients and improves glucose levels and insulin sensitivity in individuals at high risk for diabetes. These findings suggest that magnesium supplementation could be a beneficial strategy for managing glucose parameters and enhancing insulin sensitivity, indicating its potential role in diabetes prevention and management.
- Type 2 diabetes is often linked to magnesium (Mg) deficits, both extracellularly and intracellularly, with such deficiencies particularly noted in individuals with poor glycemic control. [61] Insulin and glucose levels significantly influence Mg metabolism, with intracellular Mg critical for insulin action and glucose uptake. Lowered Mg levels can impair insulin signaling pathways, exacerbating insulin resistance. The primary causes of Mg depletion in type 2 diabetes are believed to be low dietary intake and increased urinary loss. While some clinical studies suggest that Mg supplementation can improve metabolic profiles in diabetic patients, the evidence is not uniformly conclusive, indicating a need for more extensive research to establish dietary Mg supplementation as a viable public health strategy for diabetes prevention and management.
- Experimental studies and growing evidence have highlighted magnesium’s crucial role in glucose metabolism, suggesting its potential in reducing type 2 diabetes (T2D) risk. [62] Epidemiological research consistently indicates that low dietary magnesium intake correlates with a higher risk of T2D, yet results from randomized controlled trials on magnesium supplementation’s effects on glucose metabolism and insulin sensitivity remain mixed and controversial. This divergence points to a clear inverse relationship between dietary magnesium intake and T2D risk from observational studies, while clinical trial outcomes are less definitive and require further investigation to establish magnesium’s role in diabetes prevention and management.
- An article reviewed the relationship between magnesium intake and the incidence of type 2 diabetes (T2D), as well as the impact of magnesium supplementation on glucose metabolism, using data up to May 15, 2019. [63] Analysis of 26 publications involving 35 cohorts showed that higher magnesium intake correlates with a 22% reduced risk of T2D, with each 100 mg daily increase in magnesium intake lowering the risk by 6%. Further examination of 26 randomized controlled trials (RCTs) with 1168 participants demonstrated significant benefits of magnesium supplementation in reducing fasting plasma glucose, improving 2-hour oral glucose tolerance test results, fasting insulin levels, and insulin resistance scores, along with reductions in triglyceride levels and blood pressure. Trial sequential analysis confirmed the stability of these benefits, suggesting a dose-response relationship between magnesium intake and reduced T2D risk, and supporting magnesium supplementation to improve glucose parameters in individuals with T2D or at high risk.
- A study systematically reviewed and meta-analyzed randomized controlled trials (RCTs) to assess the impact of magnesium supplementation on cardiovascular risk factors associated with type 2 diabetes (T2D) in both diabetic and nondiabetic individuals. [64] The analysis, which included data up to June 30, 2016, found that magnesium supplementation significantly improved fasting plasma glucose, high-density lipoprotein, low-density lipoprotein, plasma triglycerides, and systolic blood pressure. Subgroup analysis revealed that diabetic subjects with low magnesium levels benefited the most. These results suggest that magnesium supplementation could reduce the risk of T2D-associated cardiovascular diseases, highlighting the need for future large-scale RCTs to develop comprehensive clinical guidelines.
- A case-control study conducted at Hassan II University Hospital of Fez from January 2015 to 2018 investigated the association between serum magnesium (Mg) levels and common complications, comorbidities of diabetes mellitus, and other biochemical indices in 170 patients. [65] Dividing participants into low Mg (n = 85) and normal Mg (n = 85) groups, findings revealed a strong correlation between serum Mg levels and factors such as age, sex, duration of diabetes, body mass index, hypertension, and glycosylated hemoglobin. Specifically, a negative correlation was observed between Mg levels and the presence of nephropathy, while no significant correlations were found with retinopathy, neuropathy, and macroangiopathy. The results suggest low Mg levels are associated with poor glycemic control, hypertension, and nephropathy in Type 2 diabetes patients, indicating the need for further research to solidify these findings.
- A cross-sectional study conducted over six months at the Department of Medicine, S.P. Medical College & Associated Group of Hospitals, Bikaner, aimed to investigate the association between serum magnesium levels, Type 2 diabetes mellitus (DM), and its complications among 50.4% male and 49.6% female patients with an average age of 48±18 years. [66] It was found that patients with hypomagnesemia (Mg < 1.7mg/dl) exhibited significant associations with diabetic microvascular complications, specifically nephropathy, neuropathy, retinopathy, and cardiovascular disease, but not with hypertension and cerebrovascular events. The study concludes that serum magnesium measurement is crucial for patients with uncontrolled blood sugar despite medication or insulin use, as low magnesium levels may contribute to microvascular complications of diabetes. Magnesium supplementation, being cost-effective, is recommended for patients with hypomagnesemia, particularly due to its correlation with nephropathy.
- A comprehensive review of eighteen randomized controlled trials (RCTs) investigated the impact of oral magnesium (Mg) supplementation on glucose and insulin-sensitivity parameters in individuals with diabetes or at high risk for it, revealing a beneficial effect compared to placebo. [67] For those already diagnosed with diabetes, Mg supplementation significantly reduced fasting plasma glucose. Among those at high risk of diabetes, Mg notably improved glucose levels after a glucose tolerance test and showed a trend towards reducing insulin resistance. These findings underscore magnesium’s potential in improving glucose control and insulin sensitivity, suggesting its supplementation could be a valuable addition to diabetes management and prevention strategies.
- In a study examining the effects of oral magnesium (Mg) supplementation in insulin-requiring Type 2 diabetes mellitus (DM) patients, fifty participants were randomized to receive either 15 mmol Mg or a placebo daily for three months. [68] Results showed an increase in plasma Mg concentration and Mg excretion in those receiving magnesium compared to placebo, without significant changes in erythrocyte Mg concentrations, glycaemic control (glucose and HbA1c levels), lipid profiles, or blood pressure. An analysis of patients who completed the treatment suggested a potential decrease in diastolic pressure associated with increased plasma Mg levels. However, the study concluded that three months of oral Mg supplementation increased plasma Mg concentration and urinary Mg excretion but did not significantly impact glycemic control or plasma lipid concentrations in insulin-requiring Type 2 DM patients.
- In a prospective study of 1999 Japanese adults aged 40-79 years without diabetes, followed for an average of 15.6 years, it was found that higher magnesium intake was associated with a significantly lower incidence of Type 2 diabetes. [69] The risk of developing Type 2 diabetes decreased with increasing quartiles of magnesium intake, with those in the highest quartiles showing a 33-37% lower risk compared to the lowest quartile. This protective effect was even more pronounced among individuals with insulin resistance, low-grade inflammation, or those who consumed alcohol, indicating that increased magnesium intake could significantly reduce the risk of Type 2 diabetes in the general population, particularly in individuals with specific health profiles.
H. Fights Inflammation
Magnesium fights inflammation by inhibiting the activation of inflammatory markers in the body. It plays a crucial role in the immune response by acting as a natural calcium antagonist, which helps to regulate cellular events involved in inflammation. Studies have shown that higher magnesium intake is associated with reduced levels of C-reactive protein (CRP) and other markers of inflammation in the body. This mineral’s anti-inflammatory properties are particularly beneficial in reducing the risk of chronic diseases associated with high levels of inflammation, such as heart disease, diabetes, and certain cancers.
A growing body of evidence supports the anti-inflammatory effects of magnesium:
- Magnesium deficiency in animal studies has been linked to an inflammatory response characterized by the activation of leukocytes and macrophages, the release of inflammatory cytokines, and an increase in free radicals, primarily due to elevated cellular calcium levels that prime cells for inflammation. [70] This deficiency is associated with chronic low-grade inflammation, marked by elevated levels of pro-inflammatory cytokines and acute-phase reactants, contributing to the risk of diseases like cardiovascular disease, hypertension, and diabetes. Adequate magnesium intake, on the other hand, does not significantly affect these inflammation markers. These findings underscore magnesium’s critical role in preventing chronic low-grade inflammation, highlighting the importance of magnesium-rich foods in the diet, especially in countries where magnesium deficiency is common due to inadequate dietary intake.
- Magnesium plays a crucial role in regulating metabolism, maintaining tissue homeostasis, and supporting immune functions by influencing both innate and adaptive immune cells. [71] Deficiency in magnesium can lead to heightened inflammatory responses, including increased phagocyte priming, granulocyte oxidative bursts, endothelial cell activation, and elevated cytokine levels, thereby exacerbating the body’s reaction to immune challenges. This underdiagnosed condition is linked to the development of numerous chronic diseases, with recent research emphasizing the connection between magnesium deficiency, inflammation, and the mechanisms driving these health issues.
- A systematic review and meta-analysis reviewed randomized control trials (RCTs) up to 23 November 2021 to assess the effects of magnesium (Mg) supplementation versus placebo on serum inflammatory markers. [72] After screening 2,484 papers, 17 RCTs involving 889 participants (average age: 46 years; 62.5% females) with generally low risk of bias were included. The findings showed that magnesium supplementation significantly reduced serum C-reactive protein (CRP) levels and increased nitric oxide (NO) levels, along with notable decreases in plasma fibrinogen, tartrate-resistant acid phosphatase type 5, tumor necrosis factor-ligand superfamily member 13B, ST2 protein, and IL-1. Therefore, magnesium supplementation is potentially effective in reducing various human inflammatory markers, highlighting its beneficial impact on health outcomes.
- Magnesium deficiency (MgD) is linked to various inflammatory mechanisms in the human body, including the activation of phagocytic cells, calcium channels, the NMDA receptor, and NF-κB, leading to a systemic stress response and inflammation. [73] This inflammation can further cause pro-atherogenic changes, endothelial dysfunction, and elevated blood pressure, implicating magnesium’s crucial role in the pathophysiology of several inflammatory diseases such as diabetes, asthma, preeclampsia, atherosclerosis, heart damage, and rheumatoid arthritis. The review of clinical trials and laboratory studies underscores magnesium’s potential impact on these conditions, highlighting the importance of magnesium in managing and understanding inflammatory diseases.
- A review highlights that subclinical magnesium deficiency, often resulting from low dietary intake, is a key factor predisposing individuals to chronic inflammatory stress, thereby increasing the risk of chronic diseases like cardiovascular disease and diabetes. [74] Recent findings associate deficient magnesium intakes and low serum magnesium levels with elevated serum C-reactive protein concentrations, a marker of inflammation. Correcting magnesium deficiency by achieving adequate dietary intake or serum levels can reduce inflammation indicators to normal levels. This deficiency is particularly prevalent among obese individuals and those with chronic diseases where low-grade inflammation is a known risk factor, underscoring the importance of magnesium as a critical nutrient for health and disease prevention.
- A review consolidates experimental evidence demonstrating magnesium’s role in modulating cellular processes related to inflammation. [75] In rats, magnesium deficiency quickly leads to an inflammatory syndrome marked by the activation of leukocytes and macrophages, the release of inflammatory cytokines, and an overproduction of free radicals. Altering extracellular magnesium levels impacts the inflammatory response, with increased levels reducing and decreased levels enhancing cell activation, largely due to magnesium’s function as a natural calcium antagonist affecting intracellular calcium concentrations. Potential mechanisms include phagocytic cell priming, calcium channel opening, NMDA receptor activation, and NF-kappa B activation, alongside a systemic stress response triggered by neuroendocrinological pathway activation. Magnesium deficiency’s role in exacerbating immune and oxidative stress responses links it to pro-atherogenic changes, endothelial dysfunction, and metabolic syndrome, suggesting inflammation as a key mediator in the connection between magnesium deficiency and various diseases. While further human studies are needed, these findings highlight the importance of magnesium in managing inflammation and its related disorders.
- A literature review explores the crucial role of magnesium (Mg) in immune regulation across inflammation, infection, and cancer settings, highlighting its involvement in various immune responses and its significant anti-cancer effects. [76] Mg deficiency is linked to increased baseline inflammation, oxidative stress, and various immune system complications, underscoring the importance of Mg in immune cell function, antibody synthesis, and as a cofactor in immune reactions. The review points out that while a balanced diet typically ensures adequate Mg levels, supplementation may be necessary in certain cases, though excessive amounts could impair immune function. The findings emphasize Mg’s essential role in enhancing immune responses, regulating inflammation, and its potential therapeutic efficacy, yet call for further research to elucidate its mechanisms and clinical implications fully.
- A comprehensive literature review across major databases assessed magnesium’s (Mg) role in immune regulation within contexts of inflammation, infection, and cancer. [77] It highlights Mg’s involvement in various immunological functions, such as facilitating substance P binding, promoting cell responses to lymphokines, and supporting antibody-dependent cytolysis, alongside its cofactor role in immune processes and notable anti-cancer properties. Chronic Mg deficiency is linked to increased inflammation, oxidative stress, and various immune-related complications, including lymphoma and thymus atrophy, underscoring the necessity of Mg for immune system integrity and its potential therapeutic efficacy. The review concludes that while Mg is crucial for immune function and inflammation regulation, its mechanisms and clinical implications, especially in malignancies and inflammatory conditions, warrant further investigation. Adequate dietary Mg intake is essential, with supplementation advised in certain scenarios, albeit cautiously to avoid negative immune effects.
- Despite about 60% of adults in the United States not meeting the estimated average requirement for magnesium, overt pathological conditions directly linked to magnesium deficiency are uncommon. [78] However, low magnesium status is frequently associated with various pathological conditions that involve chronic inflammatory stress. While human deficiencies are typically marginal to moderate, animal studies have shown that such deficiencies can either be mitigated or worsened by factors affecting inflammatory and oxidative stress, a notion that recent research suggests applies to humans as well. This is particularly relevant in the context of obesity, which involves chronic low-grade inflammation and is often accompanied by low magnesium status. Thus, marginal-to-moderate magnesium deficiency might significantly contribute to chronic diseases like atherosclerosis, hypertension, osteoporosis, diabetes mellitus, and cancer by exacerbating chronic inflammatory stress.
- A review highlights how magnesium (Mg) plays a crucial role in modulating cellular events linked to inflammation, with experiments showing that severe Mg deficiency in rats triggers a clinical inflammatory syndrome, including activation of immune cells, release of inflammatory cytokines, and excessive free radical production. [79] Increasing Mg levels can reduce this inflammatory response, while its reduction leads to cell activation, due to Mg’s role as a natural calcium antagonist affecting intracellular calcium levels. Mg deficiency is implicated in exacerbating responses to immune stress and contributing to a range of conditions such as hyperlipemia, atherosclerosis, endothelial dysfunction, thrombosis, hypertension, and damage from free radicals, while also facilitating the adhesion and migration of cancer cells. These findings indicate inflammation as a key factor linking Mg deficiency to various pathological states.
- A systematic review and dose-response meta-analysis, which sifted through major databases until December 14, 2020, evaluated the impact of oral magnesium supplementation on inflammatory biomarkers such as C-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-α) in adults. [80] After assessing the quality of 18 studies involving 927 participants using the Cochrane Collaboration tool and conducting subgroup analysis to pinpoint heterogeneity sources, the analysis found that magnesium supplementation did not significantly affect serum levels of CRP, IL-6, and TNF-α when compared to controls. Furthermore, dose-response assessments revealed no significant associations between the dosage or duration of magnesium supplementation and serum CRP and IL-6 concentrations. These findings do not support the hypothesis that oral magnesium supplementation beneficially impacts these specific inflammatory biomarkers in adults.
- A systematic review and meta-analysis of randomized controlled trials (RCTs) investigated the effects of oral magnesium supplementation on plasma C-reactive protein (CRP) levels, searching databases up to August 9, 2016. [81] Analyzing data from 11 studies, the meta-analysis found that magnesium supplementation did not significantly change plasma CRP concentrations overall. However, in subgroup analyses, individuals with baseline CRP levels above 3 mg/L experienced a significant reduction in CRP following magnesium treatment, suggesting a potential beneficial effect of magnesium supplementation in managing low-grade chronic systemic inflammation, particularly among those with higher levels of inflammation. This highlights magnesium’s role as a possible adjunctive therapy in inflammatory conditions.
- A study explores the link between magnesium (Mg2+) deficiency, induced by low dietary intake and the use of certain medications like diuretics, and the development of hypertension. [82] It demonstrates that higher serum Mg2+ levels and Mg2+ supplementation are associated with lower blood pressure, implicating Mg2+ deficiency in hypertension’s pathogenesis. Specifically, the research found that a Mg2+-depleted diet in mice led to increased blood pressure, without a rise in total body fluid, and elevated levels of NLRP3, IL-1β, and IsoLGs in antigen-presenting cells, indicating a direct effect of low Mg2+ on inflammation and oxidative stress pathways. These findings highlight the potential of Mg2+ supplementation and increased dietary intake as strategies to mitigate hypertension and cardiovascular disease by targeting underlying inflammatory and oxidative mechanisms.
- In a study utilizing a 5/6 nephrectomized rat model to simulate chronic kidney disease (CKD) and in vitro experiments on vascular smooth muscle cells (VSMCs), magnesium (Mg) supplementation was found to significantly mitigate systemic inflammation and oxidative stress. [83] Uraemic rats on a standard Mg diet exhibited increased levels of pro-inflammatory cytokines and oxidative stress markers, which were notably reduced with dietary Mg supplementation. Similarly, VSMCs exposed to high phosphate conditions showed decreased production of reactive oxygen species and inflammatory cytokines when incubated with increased Mg levels, highlighting Mg’s direct anti-inflammatory and antioxidative effects on vascular cells. These results suggest that Mg supplementation could be a beneficial adjunct in the clinical management of CKD patients, reducing inflammation and oxidative stress.
- A study explored the anti-inflammatory properties of magnesium isoglycyrrhizinate (MgIG), a derivative of Glycyrrhiza glabra (licorice), particularly focusing on its effects within the phospholipase A2 (PLA2)/arachidonic acid (AA) pathway in RAW264.7 macrophages. [84] It was found that MgIG significantly suppresses the activation of PLA2 and the subsequent production of AA metabolites such as prostaglandin E2, prostacyclin, thromboxane 2, and leukotrienes, which are key inflammatory mediators. Additionally, MgIG inhibited the enzymes responsible for metabolizing AA, including COX-2, COX-1, 5-LOX, and others, indicating that its anti-inflammatory effects may be attributed to the modulation of cyclooxygenase (COXs) and 5-lipoxygenase (LOX) pathways in AA metabolism. This reveals a potential novel mechanism for MgIG’s clinical use in treating inflammatory liver diseases.
Magnesium Daily Intake: How much mg of Magnesium is Enough?
The recommended daily intake of magnesium varies by age, gender, and life stage, reflecting the importance of this mineral in numerous bodily functions and aligning with the dietary reference intakes designed to prevent deficiency. Understanding the correct magnesium dosage, as outlined in the dietary reference intakes, is crucial for maintaining health. According to the National Institutes of Health (NIH), the general guidelines for magnesium dosage, which follow the dietary reference intakes, are as follows:
- Infants:
- 0-6 months: 30 mg (Adequate Intake)
- 7-12 months: 75 mg (Adequate Intake)
- Children:
- 1-3 years: 80 mg
- 4-8 years: 130 mg
- 9-13 years: 240 mg
- Teens and Adults:
- Males 14-18 years: 410 mg
- Females 14-18 years: 360 mg
- Males 19-30 years: 400 mg
- Females 19-30 years: 310 mg
- Males 31 years and older: 420 mg
- Females 31 years and older: 320 mg
- Pregnancy and Lactation:
- Pregnant teens: 400 mg
- Pregnant women: 350-360 mg (depending on age)
- Lactating teens: 360 mg
- Lactating women: 310-320 mg (depending on age)
It’s important to note that these values represent total daily intake from food, water, and, if necessary, supplements. Consuming magnesium within these recommended ranges is crucial for maintaining health and preventing magnesium deficiency. Research has shown that higher magnesium intakes, within safe limits, can offer additional health benefits, such as improved bone health and reduced risk of chronic diseases. Therefore, aiming for the higher end of the recommended intake, through a balanced diet and supplements if needed, can be beneficial.
Magnesium Supplements: Differences between Magnesium Chloride, Magnesium Hydroxide, Magnesium Oxide, Magnesium Citrate, and Other Forms
Magnesium supplements come in various forms, each with different absorption rates and specific uses. Here are some common examples:
- Magnesium Citrate: This form is magnesium combined with citric acid. It is one of the most bioavailable forms of magnesium and is often used for its laxative effect to treat constipation.
- Magnesium Oxide: Widely used for relieving digestive issues like heartburn and indigestion, magnesium oxide is also used to prevent magnesium deficiency. However, it has a lower absorption rate compared to other forms.
- Magnesium Chloride: Available in both pill form and as a topical solution, magnesium chloride is easily absorbed by the body. It can be used to raise magnesium levels and for kidney function improvement.
- Magnesium Glycinate: Known for its calming effects, magnesium glycinate is often recommended for those looking to improve sleep quality or manage stress and anxiety. It’s highly bioavailable and gentle on the stomach.
- Magnesium Sulfate: Also known as Epsom salt, it is typically dissolved in bath water to relieve muscle soreness and improve relaxation through skin absorption.
- Magnesium Lactate: This form is used by people with sensitive digestive systems because it is less likely to cause diarrhea. It’s effective for supplementing magnesium levels and is well-absorbed.
- Magnesium Malate: Magnesium malate contains malic acid, which is involved in the Krebs cycle (a series of chemical reactions used to release stored energy). It’s often recommended for managing fatigue and muscle pain.
- Magnesium Taurate: This form is a combination of magnesium and taurine, an amino acid. It is often chosen for its potential cardiovascular benefits.
- Magnesium L-threonate: Known for its ability to penetrate the brain barrier, it is suggested for improving cognitive function, memory, and for managing symptoms of anxiety.
- Magnesium Hydroxide: Magnesium hydroxide is a compound used primarily as an antacid to neutralize stomach acid and as a laxative to relieve constipation. This dietary supplement is recognized for its effectiveness in treating symptoms of indigestion, heartburn, and sour stomach. Additionally, magnesium hydroxide is used in some antiperspirant products due to its ability to interact with sweat to prevent body odor. It is available over the counter in various forms, including liquids and tablets, making it accessible for those seeking relief from gastrointestinal discomfort.
Each form of magnesium has unique benefits, and the choice of supplement may depend on individual health needs and goals. Always consult with a healthcare provider before starting any new supplement regimen to ensure it is appropriate for your specific health situation.
Magnesium Deficiency
Magnesium deficiency, medically known as hypomagnesemia, occurs when the body does not have enough magnesium, a vital mineral crucial for over 300 enzymatic reactions and various physiological functions. This deficiency can lead to a wide array of health issues since magnesium plays a key role in muscle and nerve function, maintaining a healthy immune system, keeping the heartbeat steady, and supporting bone health. It also aids in regulating blood sugar levels and blood pressure. Common causes of magnesium deficiency include inadequate dietary intake, chronic health conditions such as gastrointestinal diseases, diabetes, and excessive alcohol consumption, which can impair the body’s ability to absorb magnesium or increase its excretion.
Symptoms of magnesium deficiency are often subtle unless the levels become severely low. Initial signs can include general fatigue, weakness, loss of appetite, nausea, and vomiting. As the deficiency worsens, individuals may experience more severe symptoms such as numbness and tingling, muscle cramps and contractions, seizures, personality changes, abnormal heart rhythms, and coronary spasms. Diagnosing magnesium deficiency involves a clinical evaluation of symptoms and a confirmation through blood tests. Treatment typically involves dietary adjustments to include more magnesium-rich foods or magnesium supplements under medical supervision. Given the essential roles of magnesium in the body, preventing deficiency is key to maintaining overall health and well-being.
What is Magnesium used For?
Magnesium is an essential mineral used by the body for a wide range of functions and health benefits, including:
- Energy Production: Magnesium plays a pivotal role in converting food into energy, activating ATP, the energy molecule in the body.
- Protein Formation: It helps create new proteins from amino acids.
- Gene Maintenance: Magnesium is involved in the creation and repair of DNA and RNA.
- Muscle Movements: It is part of the contraction and relaxation of muscles.
- Nervous System Regulation: Magnesium regulates neurotransmitters, which send messages throughout the brain and nervous system.
- Electrolyte Balance: It helps regulate electrolyte balance, which is crucial for nerve and muscle function, blood pressure regulation, and hydration.
- Bone Health: Magnesium is vital for bone formation and influences the activities of osteoblasts and osteoclasts that build healthy bone density.
- Cardiovascular Health: It contributes to heart health by managing the transport of calcium and potassium across cell membranes, critical for normal heart rhythm and blood pressure control.
- Blood Sugar Control: Magnesium plays a key role in glucose and insulin metabolism, with higher magnesium intakes associated with a lower risk of type 2 diabetes.
- Mental Health: It has been studied for its role in brain function and mood regulation, including potential benefits for anxiety and depression.
- Digestion and Relieving Constipation: Magnesium draws water into the intestines, making stool easier to pass, and is often used as a natural remedy for constipation.
- Migraine Prevention: Some studies suggest that magnesium deficiency is more common in people who suffer from migraines, and supplementation may help prevent or reduce symptoms.
- Anti-inflammatory Benefits: Lower magnesium intake is linked to chronic inflammation, which is underlying many diseases. Supplementing with magnesium can reduce inflammation in certain conditions.
Magnesium supplementation can be beneficial in treating and preventing magnesium deficiency and its associated symptoms and conditions. However, it’s important to use magnesium supplements under medical supervision, especially for individuals with certain health conditions or those taking medications that might interact with magnesium.
What is Magnesium Glycinate?
Magnesium glycinate is a form of magnesium supplement where magnesium is bonded to glycine, an amino acid. This combination creates a compound that is highly bioavailable, meaning it’s easily absorbed by the body, making it one of the most effective forms of magnesium supplements available. Magnesium glycinate is particularly noted for its ability to provide the benefits of magnesium without the common side effects of gastrointestinal distress or laxative properties that other forms of magnesium supplements might cause.
It is commonly recommended for those seeking to increase their magnesium intake for various health reasons, including improving sleep quality, supporting bone health, managing stress and anxiety, aiding in muscle recovery and function, and maintaining normal nerve function. Magnesium glycinate’s enhanced absorption rate and gentle effect on the stomach make it a preferred choice for dietary supplementation, especially for individuals with magnesium deficiencies or those in need of magnesium’s therapeutic effects without gastrointestinal discomfort.
Magnesium Tablets
Magnesium tablets are a popular dietary supplement used to increase magnesium intake, an essential mineral vital for numerous bodily functions. Magnesium is crucial for over 300 enzyme reactions in the body, including DNA synthesis, muscle and nerve function, blood glucose control, and blood pressure regulation. Despite its abundance in various foods, many individuals may not consume enough magnesium through diet alone, leading to deficiencies. This shortfall is where magnesium tablets come into play, offering a convenient way to ensure adequate magnesium levels. They are particularly beneficial for individuals at risk of magnesium deficiency, including those with gastrointestinal diseases, type 2 diabetes, alcohol dependencies, and older adults.
The choice of magnesium tablets can depend on individual health needs and tolerability, as magnesium supplements come in various forms, each with different absorption rates and effects on the gastrointestinal system. For instance, magnesium citrate is known for its bioavailability and laxative effect, making it suitable for those suffering from constipation. In contrast, magnesium glycinate is often recommended for its calming effects on the brain and muscles, making it ideal for improving sleep and reducing muscle cramps without causing diarrhea. When taking magnesium tablets, it’s important to adhere to the recommended dietary allowances unless a healthcare provider advises otherwise, as excessive magnesium intake can lead to adverse effects, including diarrhea, nausea, and abdominal cramping.
Magnesium Side Effects
While magnesium is essential for health and involved in more than 300 biochemical reactions in the body, taking too much, especially in supplement form, can lead to side effects. These side effects are more common when magnesium is taken in high doses and can vary depending on the individual and the form of magnesium consumed. Common side effects of excessive magnesium intake include:
- Diarrhea: This is the most common side effect, especially with magnesium forms such as magnesium carbonate, chloride, oxide, and citrate, which have a laxative effect.
- Nausea and Vomiting: High doses of magnesium can upset the stomach and lead to nausea or vomiting.
- Abdominal Cramping: Overconsumption of magnesium supplements can cause stomach cramps and discomfort.
- Electrolyte Imbalance: Extremely high levels of magnesium can lead to an imbalance of electrolytes, specifically lowering calcium (hypocalcemia) and potassium levels (hypokalemia) in the blood.
- Low Blood Pressure: Excessive magnesium intake lowers blood pressure, which can be beneficial in some cases but problematic in others, especially if it causes symptoms of lightheadedness or fainting.
- Irregular Heartbeat: Though rare, very high magnesium levels can affect heart rhythms, leading to irregular heartbeats or arrhythmias.
- Breathing Problems: In severe cases, too much magnesium can lead to difficulty breathing.
- Lethargy: High doses of magnesium can cause drowsiness, lethargy, and a lack of energy.
The tolerable upper intake level (UL) for magnesium from supplements and medication, not including dietary magnesium, is 350 mg per day for adults and teenagers. This limit is set to prevent the risk of side effects. However, dietary magnesium, found naturally in foods, does not pose a risk for side effects and is not included in the UL.
It’s important to consult with a healthcare provider before starting any new supplement regimen, especially if you have kidney function issues or take medications that could interact with magnesium supplements.
















